Peripheral Arterial Disease
- Home
- Peripheral Arterial Disease
Peripheral Arterial Disease
Introduction
Arteries are blood vessels that carry oxygenated blood from the heart to all parts of the body. The arterial wall has three layers – outer adventia (connective tissue), middle media (muscular) and inner intima (smooth layer). When cholesterol gets deposited between the middle and inner layer it is called as a plaque and causes a bump that results in narrowing of the artery and making the inner smooth layer rough. This causes reduction in flow and the blood cells start sticking to the inner layer that has become rough and results in formation of clots.

The blood supply to the organ supplied reduces (ischemia) and this results in either compromise in function or damage to the organ.
| Organ (Artery name) | Compromised function | Damage |
| Heart (Coronaries) | Chest pain – Angina Shortness of breath with exertion | Heart Attack or infarct (AMI) |
| Brain (Carotid, Vertebral) | TIA – Transient ischemic Attack Hypoperfusion – Blackout | Stroke – Paralysis |
| Kidneys (Renal) | High BP | Renal failure |
| Extremities – Arms, Legs (peripheral arteries) | Leg pain on walking – claudication Ischemic nerve – Rest pain | Damage – Ulcers, Gangrene |
Causes
This occurs more often in older people (> 60 years) but may occur in younger people if they have bad family history or risk factors such as high BP, diabetes (poorly controlled or long duration), high Cholesterol, Uric acid, Smoking or tobacco use, or have thickening of blood due to high homocysteine or disorder of the blood that makes it sticky (pro-thrombotic).
It is important to note that disease of arteries to different organs may be present at the same time to varying extent and that presence in one area indicates possibility of involvement of other areas too. Involvement of leg arteries is more common than arm arteries. There is an overlap of around 60% between the arteries of the heart, brain and legs getting affected at the same time.
Symptoms
 When the blood supply to the muscles is reduced, one gets pain in that muscle after it is used. Hence depending on which artery is narrowed one may get pain in the foot (lower leg arteries), calf (thigh arteries) or buttocks (arteries above groin). This pain comes on walking, reduces after stopping and recurs on further walking. It is a cramp like pain (Claudication) and occurs because the muscles swell up because of accumulation of lactic acid. It does not occur on standing and one does not need to sit for the pain to go away. If one does not walk much, the pain does not occur, and one remains unaware of the narrowing of the artery until it becomes very severe. The distance one can walk before pain occurs is called “Claudication distance” and the distance at which it becomes unbearable and one is forced to stop is called “Absolute Claudication distance”. Besides severity of narrowing, this distance become shorter if one walks fast or climbs up a slope or stairs where the effort is more. The risk of loss of limb is low in patients with claudication who are found to have a reduction in life span by around 10 years.
When the blood supply to the muscles is reduced, one gets pain in that muscle after it is used. Hence depending on which artery is narrowed one may get pain in the foot (lower leg arteries), calf (thigh arteries) or buttocks (arteries above groin). This pain comes on walking, reduces after stopping and recurs on further walking. It is a cramp like pain (Claudication) and occurs because the muscles swell up because of accumulation of lactic acid. It does not occur on standing and one does not need to sit for the pain to go away. If one does not walk much, the pain does not occur, and one remains unaware of the narrowing of the artery until it becomes very severe. The distance one can walk before pain occurs is called “Claudication distance” and the distance at which it becomes unbearable and one is forced to stop is called “Absolute Claudication distance”. Besides severity of narrowing, this distance become shorter if one walks fast or climbs up a slope or stairs where the effort is more. The risk of loss of limb is low in patients with claudication who are found to have a reduction in life span by around 10 years.
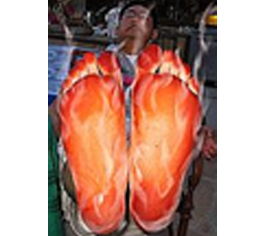 When the narrowing is very severe, the blood supply to the nerve in that area gets compromised and it results in a burning type of pain and is present when the person is resting in the lying down position with the limb flat on the bed. This is called “Rest pain”. It is relieved when the limb is placed in the dependent position as the gravity helps more blood reach the nerve. The foot is usually red in colour but cold. On elevation it becomes pale due to reduction in blood supply.
When the narrowing is very severe, the blood supply to the nerve in that area gets compromised and it results in a burning type of pain and is present when the person is resting in the lying down position with the limb flat on the bed. This is called “Rest pain”. It is relieved when the limb is placed in the dependent position as the gravity helps more blood reach the nerve. The foot is usually red in colour but cold. On elevation it becomes pale due to reduction in blood supply.
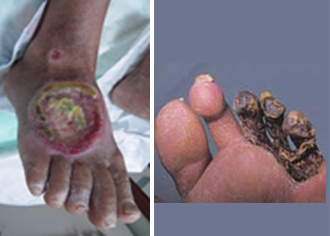 If one gets any injury at this stage eg while trimming nails, shoe bite, thermal injury or any infection, the wound does not heal and may progress to gangrene when there is death of the tissue. The area is very painful and this pain is difficult to control. These conditions ie rest pain, non-healing wounds or gangrene are called “Critical Limb Ischemia” and involve a high risk of loss of limb or life.
If one gets any injury at this stage eg while trimming nails, shoe bite, thermal injury or any infection, the wound does not heal and may progress to gangrene when there is death of the tissue. The area is very painful and this pain is difficult to control. These conditions ie rest pain, non-healing wounds or gangrene are called “Critical Limb Ischemia” and involve a high risk of loss of limb or life.
Diagnosis
 A detailed history helps the Vascular Surgeon predict which artery is affected and by looking at the colour, temperature of the limb as well as feeling the pulsations, the doctor is able to clinch the diagnosis.
A detailed history helps the Vascular Surgeon predict which artery is affected and by looking at the colour, temperature of the limb as well as feeling the pulsations, the doctor is able to clinch the diagnosis.
Further information about the extent of the disease is obtained by measuring the blood pressure in the leg arteries (at the ankle) and comparing them with those in the arm (brachial). This is called “Ankle-Brachial Index (ABI)” and is very useful in not only identifying the severity of the blockage but also in evaluation progress of the disease and response to treatment. Additional information is obtained by performing a “Exercise Stress Test for the Legs” where the drop in ABI with specific controlled exercise along with time for recovery is looked at.
More information is obtained by performing Arterial Doppler Ultrasonography. If necessary, an angiography can be performed to get a map of the arterial disease to plan treatment for restoring the blood supply. Angiography can be done in a non-invasive way using MRI (for calcified arteries) or CT scan (for non-calcified arteries with normal renal function) or invasive way by puncturing the artery and injecting dye (contrast) or Carbon Dioxide ie DSA (Digital Subtraction Angiography). In this technique the bone is subtracted so that only the arteries are seen clearly.
Treatment
Treatment starts by prescribing medications to thin the blood (anti-platelets), dilate the blood vessels, slow down progress of arterial disease (Clostazol) and control the risk factors (cholesterol, diabetes, uric acid, vitamin deficiency, etc).
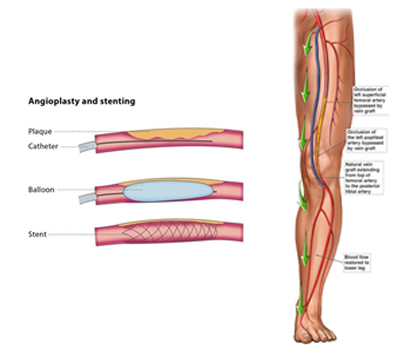 Depending on the severity of symptoms and extent of the disease the doctor may offer various options like treating the disease with only medication and walking exercise, or adding endovascular treatment like angioplasty + stenting, or open surgery like cleaning the artery (endarterectomy) or bypassing the blockage and joining a good artery above to a good artery below or using a combination of endovascular and open surgery.
Depending on the severity of symptoms and extent of the disease the doctor may offer various options like treating the disease with only medication and walking exercise, or adding endovascular treatment like angioplasty + stenting, or open surgery like cleaning the artery (endarterectomy) or bypassing the blockage and joining a good artery above to a good artery below or using a combination of endovascular and open surgery.
At times if the disease is too extensive or patient not fit for any intervention, he may advise using a Art- Assist pump, special Prostaglandin drip infusion treatment, stem cells. At times amputation may be advised to save the life by sacrificing the limb.


