Lymphedema
- Home
- Lymphedema
Lymphedema
Introduction
 Lymph is the formation of tissue fluid that takes place after tissues have extracted nutrients from the oxygen rich arterial blood that is returned as deoxygenated blood containing waste products through the veins. Lymphatic fluid is rich in proteins and is drained by the body through the lymphatic channels. These drain into the lymph nodes that are located near the joints and act as filters to deal with organisms that cause infection in the tissues. After filtering, the lymph nodes pass the lymph towards the heart through the lymphatic duct that finally empties in the L) subclavian vein.
Lymph is the formation of tissue fluid that takes place after tissues have extracted nutrients from the oxygen rich arterial blood that is returned as deoxygenated blood containing waste products through the veins. Lymphatic fluid is rich in proteins and is drained by the body through the lymphatic channels. These drain into the lymph nodes that are located near the joints and act as filters to deal with organisms that cause infection in the tissues. After filtering, the lymph nodes pass the lymph towards the heart through the lymphatic duct that finally empties in the L) subclavian vein.
Lymphedema is the accumulation of lymphatic fluid in the tissues that results in swelling of the affected part. It is more common in the legs than the arms.
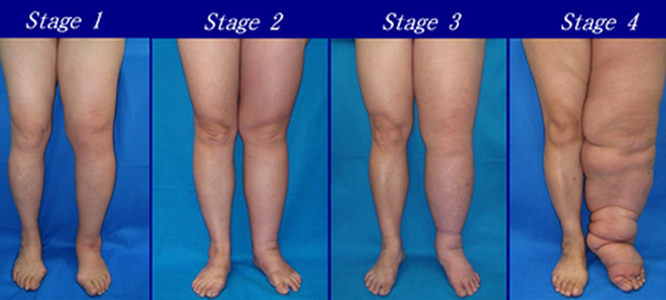
Stage 1
In the initial stages the swelling is soft, pits on pressure and is amenable to reduction with gravity and compression.
Stage 2
In the later stages, the protein in the fluid sets and hardens, does not pit on pressure (non-pitting) and results in fibrosis within the soft tissue.
Stage 3
As the condition worsens, the skin also gets affected and starts appearing like an Orange peal (Peu d’orange). It loses its ability to fight infection and gets prone to repeated bacterial and fungal infection.
Stage 4
The accumulated fluid also causes the tissue to expand and bulge developing folds. In advanced stages it is also referred as Elephantiasis. Use of the limb gets affected as it becomes very heavy and difficult to lift or move.
Causes
Lymphedema is the accumulation of lymphatic fluid in the tissues that takes place if
1 More tissue fluid is formed due to
- (a) Obstruction at the venous end (venous thrombosis) or
- (b) If there is infection (wounds or fungal infection).
2. Drainage is impaired because of problems with lymphatics or draining lymph nodes due to
- (a) Faulty development (present in childhood but may become apparent later after it increases) also called Primary Lymphedema
- (b) Damage – minor or major trauma
- (c) Removal – as part of cancer surgery (eg post mastectomy lymphedema of the arm)
- (d) Blockage following infection with Filarial worm.
Symptoms
If the cause is due to Filarial infection, there is usually a history of fever with chills along with episodes of redness in the legs. The fever occurs when the adult worm residing in the lymph nodes releases its larvae (Microfilaria) within the blood stream. This is usually common in some areas and the worm gets introduced in the body through a mosquito bite.
Non-filarial causes may give a history of minor twisting injury, major injury, infection, major surgical removal of tissue, cancer surgery with removal of lymph nodes or involvement of draining veins, Deep Vein Thrombosis (DVT).
In the initial stages, there is only swelling, heaviness or tightness. This reduces easily with elevation or compression bandaging.
As the disease progresses there is progressive increase in the swelling with appearance of bulges and folds or creases. The swelling also gets harder and does not reduce with elevation.
Skin initially swells up and shows “orange peal” appearance. Later on it starts getting harder and becomes rough following damage to sweat and sebaceous glands. It is now prone to infection due to fungi or bacteria that in turn causes infection to spread (cellulitis), more fluid to form and worsening of condition.
Diagnosis
Detailed history taking is mandatory and efforts to look for enlarged lymph nodes draining the affected limb. Efforts must be made to identify and irradicate fungal infection in the folds, creases or web spaces.
During the acute episode of fever, microfilaria may be seen in blood or the patient may test positive for Filarial antigen.
Lymphoscintigraphy is performed by injecting radio labelled sulphur colloid or albumin into the foot or hand on both sides and images taken at specific intervals to look for drainage proximally, appearance of lymph nodes and drainage above from the lymph nodes.

It is also a good practice to check the Veins for high pressure due to reflux (Venous doppler for incompetence) and obstruction (Venous Doppler for DVT and / or MR venography).
Treatment
Treatment offered depends on the stage of the disease and involves use of different modalities in various permutation and combination
- Customary to give a 3-6 monthly course of anti-protozoal (1 day – T. Zentel) and anti-microfilarial medication (Hetrazan / Banocide given for 21 days
- Microflavinoid (Daflon) may help improve venous drainage and help reduce tissue fluid formation
- Limb elevation – raise foot end of bed while lying down for legs or rest upper limb on pillows for post-mastectomy lymphedema.
- Regular oil massage distal to proximal along with exercises to open of lymphatics and improve drainage.
- Look after the skin and use moisturizers taking care not to cause maceration of the skin.

- Use of Lymphapress compression pump and sleaves to reduce fluid and force drainage. These may have different number of chambers (4, 6, 8, 12). The chambers are inflated distal to proximal thereby milking the leg in regular cycles. Pressure is applied up to 120mm of Hg.
- Use of compression bandaging (multilayer) with or without compression pump to help reduce the swelling.
- Use of Class III graduated compression stockings once the swelling is reduced or fails to reduce.
- Tissue reduction surgery if there is large amount of swelling and folds.
- Surgery to improve drainage –
- (a) Lympho-nodal bypass
- (b) Insertion of multiple silastic drainage tubes to cross the level of lymph node obstruction.


